The Sleepy Tooth Guide to Pediatric Sedation
Medically Reviewed by Mohammad Aghiad Kandar, DDS
Child dental sedation is the use of medication to help children feel calm, comfortable, and safe during dental procedures. Here's a quick overview of your main options:
| Sedation Type | How It's Given | Child's State |
|---|---|---|
| Nitrous oxide (laughing gas) | Inhaled through a mask | Relaxed, awake |
| Oral conscious sedation | Liquid or pill by mouth | Drowsy, cooperative |
| IV (deep) sedation | Injected into a vein | Deeply sedated |
| General anesthesia | Inhaled or IV | Fully unconscious |
Young children often struggle to sit still or manage fear during dental work. That's completely normal. And sometimes, no amount of distraction or reassurance is enough to get necessary treatment done safely.
That's where sedation comes in.
It isn't just for major procedures. Pediatric dentists may recommend sedation for:
- Children with significant dental anxiety
- Kids who need extensive or lengthy treatment
- Children with special needs or developmental disabilities
- Very young children who can't cooperate with treatment
The right type of sedation depends on your child's age, health, anxiety level, and the procedure involved. Safety guidelines from the American Academy of Pediatrics (AAP) and the American Academy of Pediatric Dentistry (AAPD) set clear standards for who can administer sedation, what monitoring is required, and how emergencies are handled.
I'm Mohammad Aghiad Kandar, DDS, a dentist at UNO DENTAL SAN FRANCISCO with over 15 years of experience, including focused continuing education in sedation monitoring, and I've helped many families navigate the topic of child dental sedation with confidence. In the sections below, I'll walk you through everything you need to know, from sedation levels and safety protocols to preparation and recovery.
Easy child dental sedation word list:
Understanding the Levels of Child Dental Sedation
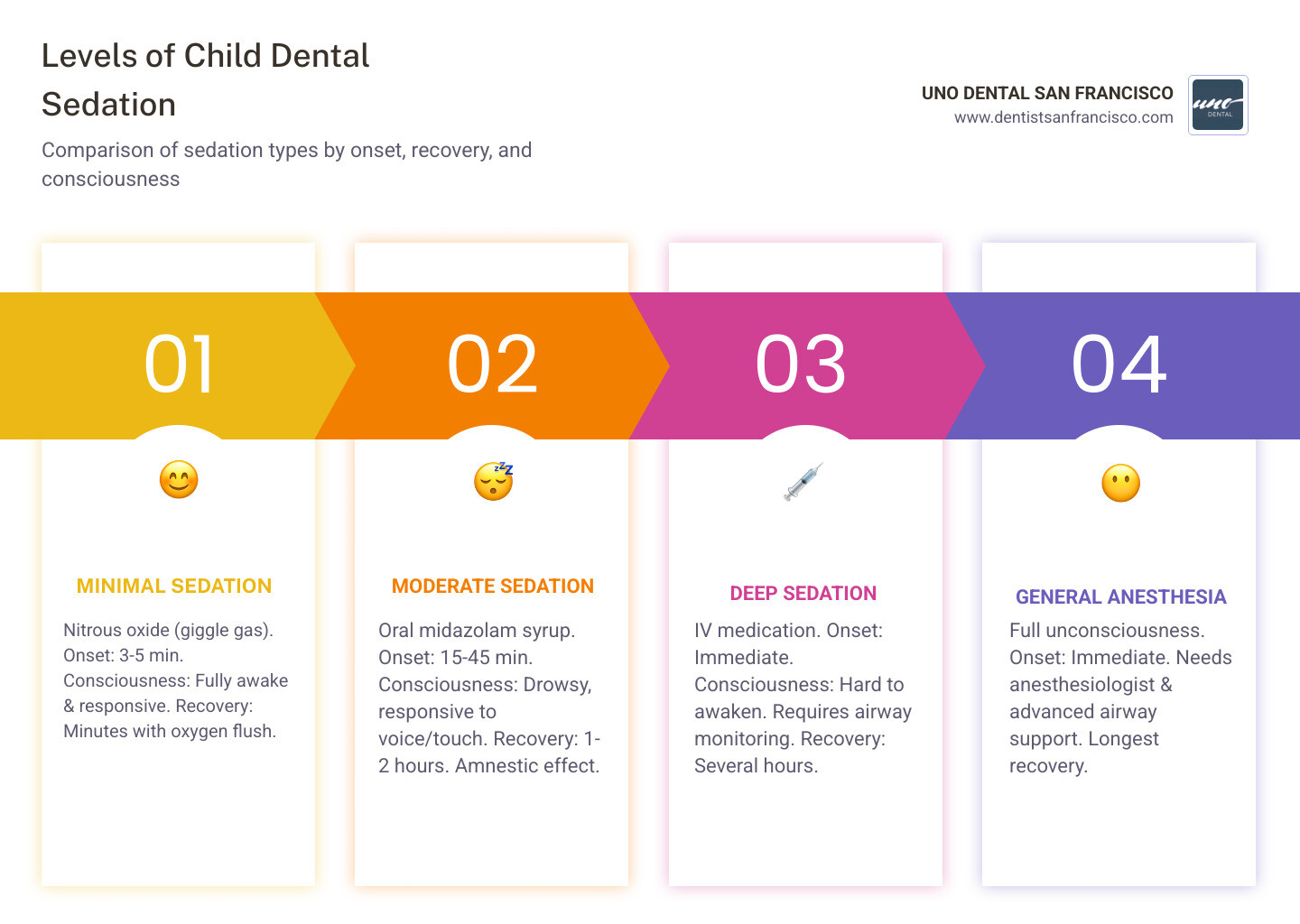
When we talk about child dental sedation, it is important to understand that it exists on a continuum. It isn't a "one-size-fits-all" switch; rather, it is a range of relaxation that we tailor to your child’s specific needs. At UNO DENTAL SAN FRANCISCO, we prioritize the least invasive method that will safely allow us to provide high-quality care.
The journey usually begins with Nitrous Oxide, often called "giggle gas" or "laughing gas." This is the most common form of minimal sedation. Your child breathes a blend of nitrous oxide and oxygen through a small mask (sometimes called an "elephant nose"). Within 3 to 5 minutes, they feel silly, lightheaded, and relaxed. The best part? The effects are fully reversible. Once we switch to pure oxygen at the end of the visit, the gas is flushed out of their system almost immediately, and they can go back to their normal activities.
We also practice iatrosedation, which is a natural, non-pharmacological approach. This involves using a calm voice, gentle mannerisms, and a welcoming environment to induce relaxation without any medication at all. For many children, this combined with nitrous oxide is the perfect recipe for a "twilight sleep" experience where they remain awake but completely unbothered by the sounds or sensations of the dental office.
To learn more about how these methods keep your child comfortable, you can read our guide on what is conscious sedation.
Oral Conscious Sedation: A Common Choice for Child Dental Sedation
If nitrous oxide isn't enough to help a very anxious child, we may move to oral conscious sedation. This is classified as moderate sedation. We typically administer this in the form of a liquid, such as midazolam syrup, which some children say tastes a bit like chocolate milk.
Unlike general anesthesia, your child is not "out." They remain conscious and can respond to verbal commands or a gentle touch. However, they will be very drowsy and may even drift into a light sleep. One of the primary benefits of this method is its "amnestic" effect—most children have little to no memory of the actual procedure, which helps prevent the development of future dental phobias.
This enteral administration (meaning it is swallowed) takes about 15 to 45 minutes to take effect. During this time, we closely monitor your child's vitals to ensure they are responding perfectly to the medication. For a deeper dive into this specific option, see our article on dental sedation for children.
Deep Sedation and General Anesthesia in Child Dental Sedation
For the most complex cases—such as a toddler needing multiple root canals or a child with severe developmental disabilities—Deep Sedation or General Anesthesia may be the safest route.
- Deep Sedation (IV Sedation): This is the parenteral route, where medication is delivered directly into a vein. Your child will be in a much deeper state of relaxation and will likely not be easily awakened until the medication wears off.
- General Anesthesia: This is reserved for situations where it is unsafe for the child to move at all. The child is fully unconscious and requires advanced airway management.
While many procedures can be done in a high-tech office like ours, some cases may be referred to hospital-based dentistry or specialized surgical centers. Regardless of the setting, the goal remains the same: ensuring the child receives necessary care without trauma. You can find more details on our sedation dentistry in San Francisco services page.
Safety Standards and AAP/AAPD Guidelines
Safety is the foundation of everything we do. In 2019, the American Academy of Pediatrics (AAP) and the American Academy of Pediatric Dentistry (AAPD) updated their clinical guidelines to make pediatric sedation safer than ever before.
One of the most critical updates requires that for deep sedation or general anesthesia, there must be at least two professionals in the room who are trained in advanced life support. One professional performs the dental procedure, while the second—an independent observer—is dedicated solely to monitoring the child’s vitals and maintaining their airway.
During the procedure, we use advanced technology to keep a constant watch on your child:
- Pulse Oximetry: Monitors the oxygen levels in the blood.
- Capnography: Measures the carbon dioxide in every breath, which is the "gold standard" for detecting breathing changes before they become a problem.
- Precordial Stethoscope: Allows the provider to listen directly to the heart and lung sounds.
These protocols ensure that even if a child drifts into a deeper level of sedation than intended (since sedation is a continuum), the team has the "rescue skills" and PALS (Pediatric Advanced Life Support) certification to manage the situation immediately. For those who want to read the technical details, you can view the full scientific research on pediatric sedation guidelines.
Qualified Professionals and Monitoring Protocols
Knowing who is taking care of your child is vital for your peace of mind. Pediatric dentists undergo an additional 2 to 3 years of residency training after dental school, which includes specific training in child dental sedation.
However, for deeper levels of sedation, we often collaborate with:
- Dentist Anesthesiologists: Professionals who completed a 3 to 5-year anesthesiology residency.
- Certified Registered Nurse Anesthetists (CRNAs): Specialized nurses with advanced anesthesia training.
- Dental Sedation Assistants: Trained staff who help monitor vitals but do not administer the medication.
Before you agree to any procedure, we encourage you to discuss all options with our team to feel empowered and informed.
Preparing Your Child for a Sedation Appointment
Preparation starts at home, and the most important rule is the "NPO" status—which means "nothing by mouth." Because sedation can sometimes cause nausea, having an empty stomach is essential for preventing aspiration (where stomach contents enter the lungs).
We follow the ASA (American Society of Anesthesiologists) fasting guidelines:
- 2 Hours Before: Clear liquids only (water, apple juice, Pedialyte).
- 4 Hours Before: Breast milk only.
- 6 Hours Before: Light meal (toast and clear liquid) or infant formula.
- 8 Hours Before: A full or fatty meal (anything fried or containing meat).
Beyond fasting, we need a complete medical history. Does your child have asthma? Have they had a recent cold or ear infection? For children with unique needs, we provide specialized care; you can learn more about our special needs kids dentistry approach.
On the day of the appointment, we will perform a final physical examination and review the informed consent forms with you. Your calm attitude is contagious—if you stay relaxed and positive, your child will likely feel the same way.
Recovery and Aftercare: What to Expect at Home
Once the procedure is over, your child will spend some time in our recovery area. They might be "loopy," sleepy, or even a little irritable as the medication wears off. This is completely normal.
Post-operative instructions for home:
- The Car Ride Home: If your child is still in a car seat, we recommend having two adults in the car—one to drive and one to sit next to the child to ensure their head doesn't flop forward, which could block their airway.
- Diet: Start with sips of water or clear liquids. If they handle that well, move to soft foods like yogurt, applesauce, or mashed potatoes. Avoid anything sharp or crunchy for 24 hours.
- Activity: No running, jumping, or swimming for the rest of the day. Let them be a "couch potato" and watch their favorite movies.
- Pain Management: We will provide specific instructions on using children's Tylenol or Motrin to manage any soreness.
Managing the aftermath is often about managing the child's mood. For tips on this, check out our guide on managing dental anxiety in children.
When to call us immediately:
- A fever over 102°F.
- Difficulty swallowing or persistent vomiting.
- Excessive bleeding that doesn't stop with pressure.
- Any breathing concerns (in which case, call 911 first).
We provide a 24-hour contact number for all our sedation patients because we want you to feel supported every step of the way.
Frequently Asked Questions about Pediatric Sedation
Is child dental sedation safe for my toddler?
Yes, when administered by qualified professionals following the 2019 AAP/AAPD guidelines, child dental sedation is very safe. We perform a thorough health screening to ensure your toddler is a good candidate. For very young children, we often use the mildest form possible to achieve the necessary results.
How long does it take for dental sedation to wear off?
It depends on the type. Nitrous oxide wears off in about 5 minutes. Oral conscious sedation usually leaves a child feeling drowsy for 30 minutes to an hour after the procedure, with some residual sleepiness for the rest of the day. Deep sedation may have a longer recovery period of several hours.
What should I do if my child has a cold before the appointment?
Please call us! If your child has a fever, a heavy cough, or a very runny nose, we will likely need to reschedule. A clear airway is essential for safe sedation, and respiratory infections can increase the risk of complications. We recommend your child be symptom-free for at least two days before the procedure.
Conclusion
At UNO DENTAL SAN FRANCISCO, we believe that every child deserves a healthy smile without the weight of dental trauma. By utilizing high-tech monitoring, following the strictest safety guidelines, and offering a holistic, patient-centered approach, we make child dental sedation a safe and positive experience for families in San Francisco.
Whether your child needs a simple filling with "giggle gas" or more extensive work under the care of an anesthesiologist, we are here to provide individualized treatment under one roof. Our San Francisco practice is dedicated to making every visit comfortable, safe, and stress-free.
Ready to give your child a positive dental experience? Schedule a pediatric dental visit with us today and discover the UNO DENTAL difference.